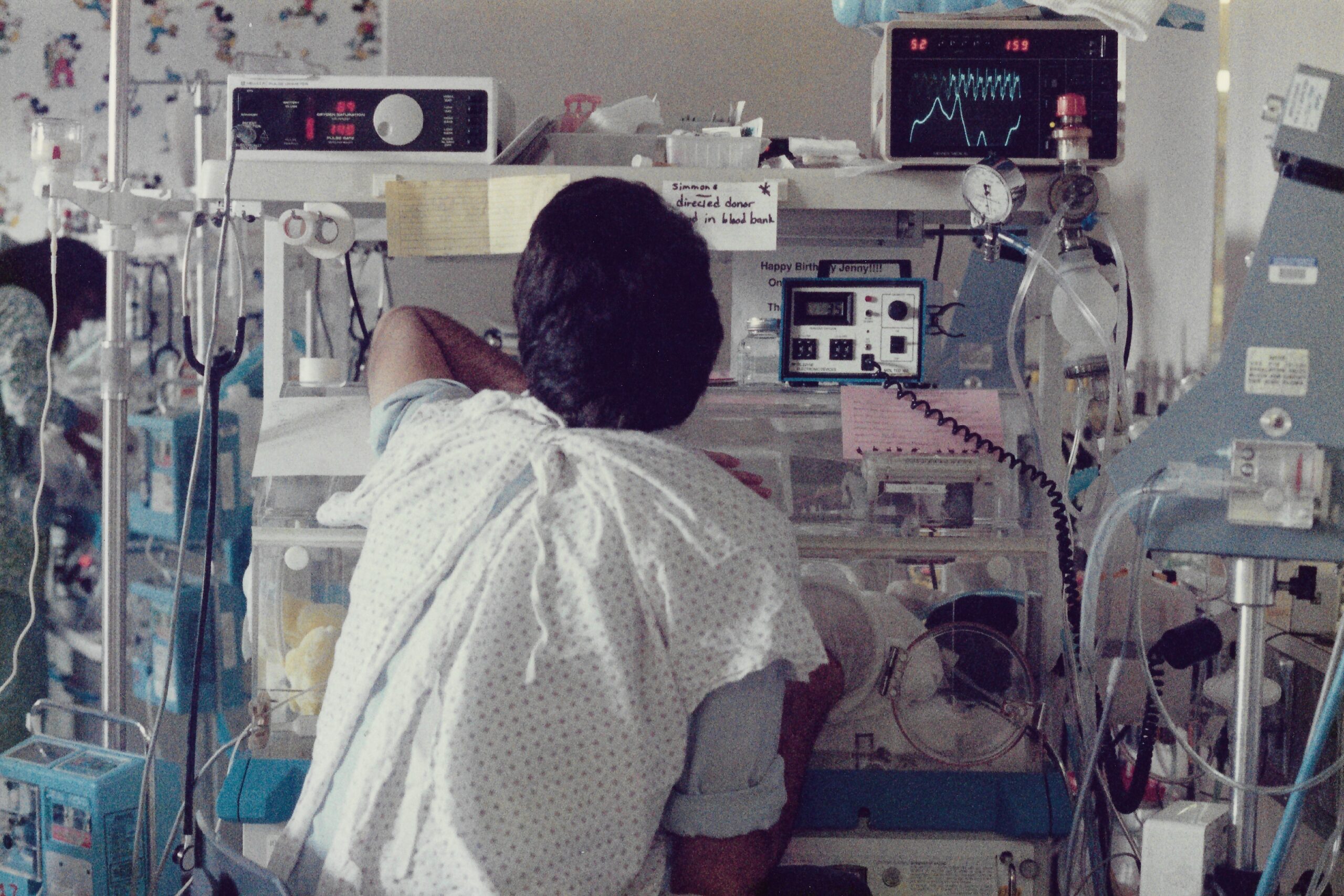
Can you tell us about your NICU experience?
Thank you so much for asking! I was surprised to get pregnant. Thirty plus years ago no one knew what PCOS (polycystic ovarian syndrome) was and I am pretty sure I had it. My cycle was all over the place, and I could not get an OBGYN to listen to my concerns. When I did get pregnant, I could not get the OBGYN practice to listen to my concern about being pregnant, as they told me for weeks that I was not. Turns out I was! From there, I was sick all day every day. At 24 weeks I was scheduled to speak at a conference in New Orleans. I lived in Washington DC at the time. I had an ultrasound before that trip, and I remember the ultrasound tech saying that the baby was awfully low. I absorbed it as concern, but there was no follow up. I realized in New Orleans that amniotic fluid was leaking. I thought about going to the emergency department there, but I could not imagine delivering there alone. I decided to get back on the plane, walk through the Atlanta airport where I saw my parents (this was the only time my parents saw me pregnant), and to fly on to DC. I called the OBGYN practice repeatedly when I got back and was told “oh it’s probably nothing.” After 24 hours of this, they told me to come in where it became very clear that I was in active labor. I remember that everyone on staff there was gray in the face. They had me walk—walk!—across the street to George Washington University hospital. I wondered if I would drop the baby right in the street.
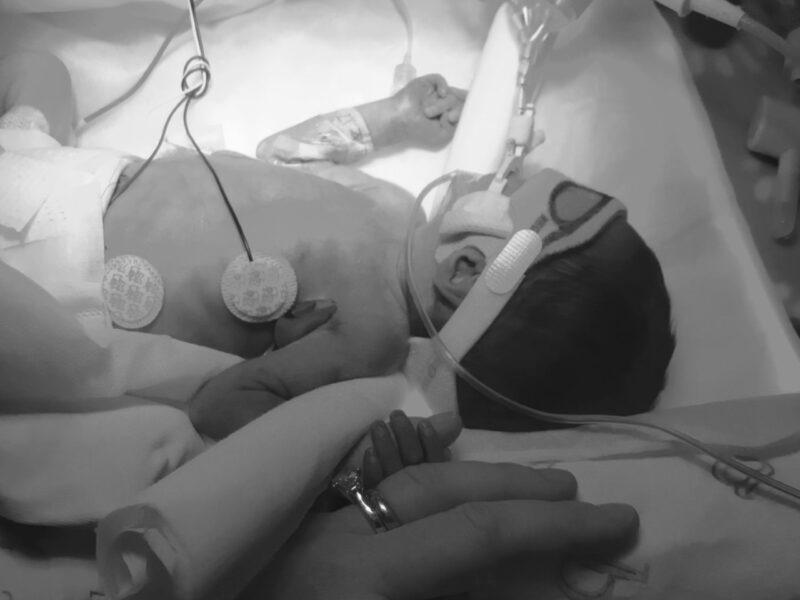
I was in active labor. I remember my best friend and her mother came to see me. I was on the phone with my parents telling them what was happening, when my water broke. I found out later that this was very traumatizing for my parents, as they had had two preemies. I delivered at 26 weeks. I bled out and hallucinated. My daughter made a kitten sound and was whisked off to the NICU. She had had a hypoxic brain injury that resulted in a bad brain bleed. She was on a ventilator off and on for weeks. On the second day of her life, her neonatologist told us that she was going to die. My husband, our friends and I surrounded her and told her that she could go, if that is what she needed to do, and that we would always love her. We sang to her. We told her that if she could stay with us, we would take her to the ocean. Her Auntie Nancy (to whom I have dedicated my book) promised a trip to Paris when she was 16. Unbelievably, she opened her eyes and decided to live. Her neonatologist told her that he believed that we had pulled her out of the grave. She had serious jaundice. There is so much waiting in the NICU! Every wait was terrifying.
I first held my daughter when she was 17 days old. Almost immediately, she was near death from sepsis on our wedding anniversary. There were many ups and downs during her 100 day stay in the NICU, including sepsis, three brain surgeries, ventilation and re-ventilation, and retinopathy of prematurity. When she finally received a VP shunt at almost two months old, it was as if her lights turned on. We began to see a living baby for the first time and to think that maybe she would come home whole. I was aware of love and laughter in the unit, as well as the daily terror. It is from this that I wrote We Are Always With You. Having a baby is a love story. You think that having a baby is a romantic comedy. With a preemie, you get the ticket to the horror or medical mystery film that keeps repeating like “Groundhog Day.”
What was the hardest part about your NICU stay? Did you learn anything about yourself?
The hardest part about the NICU was having absolutely no control and feeling helpless. Surfactant was in clinical trials at Johns Hopkins Medical Center in Baltimore, an hour away from where we lived, and I could not get my daughter into the trial. I learned in therapy that my intense shame response was from a family-of-origin that is all about shoulds and shaming. I didn’t feel that I could do anything right, no matter what I did. Having a baby early was just wrong and shameful, and I should have done something different. Therapy was life changing. My husband was suicidal. We did couples therapy and I told him that I would carry him for as long as I could, and that he also needed to do his internal work. The NICU is not a good place for religious people who think that God will keep promises about everything. Something that helped tremendously was teaching myself how to reach medical charts and the machinery. Here I am, Clinical Mommy. I decided I was part of the medical staff. I was welcomed into that role, and the staff thought I was crazy. I felt crazy.
How would you describe the period immediately after your daughter was discharged from the NICU?
I was both elated and terrified when my daughter was discharged from the NICU after 100 days. She went home with an apnea monitor. Without that, I don’t think I would ever have slept. That was the beginning of my awareness of NICU PTSD. The shoe that’s always threatening to drop. She had another surgery for a hernia a month after she came home, and I was re-traumatized. I also had the pleasure and wonder of becoming a parent. I got to watch and hear and touch her all the time. I talked and sang to her all the time. I put different spices under her nose to wake up her brain. I read to her all the time. Her first book was The Scarlet Letter. She didn’t have OT until she was 2. I wish all of her services had continued when she left the NICU. Truth be told, I checked on my daughter’s breathing every night until she was 7 years old.
How did your experience with your 26 weeker, shape your experience with your 35 weeker?
The pregnancies were very similar. Again, I threw up all day throughout the pregnancy, although a little less each day. You take a win anywhere you can get it. I thought of pregnancy as something to endure and hopefully, the baby and I would live. I didn’t have a sense of doom, as I had in the first pregnancy. I took insulin for gestational diabetes and spent more than four months on bed rest. Every day that I was on bedrest was awful. I had just started my PhD, and I had to postpone it. I had a psychotic babysitter who blamed me for how the pregnancy was going. My friends from Washington, DC came to help, but not family. At the same time, I was filled with joy that my son was inside of me, not inside of an isolette. He and I had long conversations in that bed. I remember calling the NICU in Minneapolis at 25 weeks asking about their protocols. I was anxiety-filled, and the person in the NICU could not understand why I was asking these things. When I got to 27 weeks, the hysteria settled down. When my son was born by unexpected but planned C-section at 35 weeks, I was very relieved. Someone else was in control of the birth, not me. It was an absolute wonder to hear my baby cry loudly. In my very first conversation with him, I told him “I am your mother. It is such a pleasure to meet you. Your job is to live.” He has the word “Live” tattooed on his arm. This time, he was in the special care nursery for eight days, rather than in the high-risk NICU. He was not on a ventilator. Another win. I understood the place. There were fewer surprises and upsets. While I was on high alert for him, the course was more straightforward. Again, it was hard being away from him. I would march into the unit every day to see him, despite my mother’s pleas to rest because of the C-section. I told her that there was nothing on this earth that would keep me from that boy. When you become a Clinical Mommy, you have some Tiger Mommy in you. It was very nice to have a baby who was not a science project to figure out.
Working in medical family therapy, how do you help your families process, grieve and heal from having a traumatic birth and/or a NICU stay?
The most important thing that happens when I am working with someone with a traumatic birth and /or a NICU stay, is to hear that person’s reproductive story. This might be the first time that person has had the opportunity to tell the entire story in their own words. It might include the details of physical sensations, sounds, sites, smells, as well as the emotions of helplessness, anger, disbelief, embarrassment, disappointment, shame, and guilt. I do a lot of normalizing with people. It is normal to feel whatever you feel when a traumatic birth has happened. This is an unexpected, extraordinary event that you and others around you have never experienced. It is different than the easy delivery with a fully-cooked baby. When a baby is in the NICU, I normalize the longing for being with the baby all the time, and the guilt and shame of not having carried to term. I refrain from “at least” (for example, at least the baby is alive, at least you’re not pregnant anymore). ”At least” comments completely invalidate the depth of what a person is going through. Others attempt to make everything right and nice and tidy. Premature delivery is messy and disorienting. The NICU is not nice and tidy. It is one step forward, three steps back. Like the infertility journey, the roller coaster is definitely present in the NICU. I emphasize the importance of trusting one’s intuition. When appropriate, I will offer parts of my story that indicate a common understanding of the disbelief that a birth has gone this way, and that a baby is struggling. I normalize the fear and uncertainty of the future. I bring tremendous compassion to my work, because trauma requires patience and compassion. I do a lot of EMDR (Eye Movement Desensitization and Reprocessing) in my work, to help mind and body to shift or de-intensify traumatic experiences. Cognitive behavioral therapy is helpful in reframing what happened. For example, the birth was awful and it’s over now. That is somewhat true. EMDR helps those words to actually feel true. And lots of hugs, be they virtual or in person.
Tell us about your book We Are Always With You, my love story for preemies and preemie parents.
I wrote We Are Always With You as a way of understanding what my daughter and I had lived through. When she was two years old, I started showing her pictures of the NICU, to explain to her how extraordinary it was that she was alive. I often talked about the people in the unit and how much the staff loved her and cared for her parents. She would call the pictures her “sick pictures”. She became interested in being a health care provider from a very young age. When I was on bedrest with her brother, she would examine me with her stethoscope and doctor kit, again, more normalizing. Some pregnancies are like this one. Like many traumatized NICU parents, it is difficult to relive the experience. We tend to avoid it. I encourage people to tell their children their NICU story , because it is real and because it is the extraordinary story of that child and the people who loved the child and the parents. Everything about this book has been about finding a way to help others to heal. And to honor my babies.
Is there anything else that you would like to share?
We learn from stories. It is important to tell the stories of our lives. My book is intended to help parents to craft a narrative for their babies and themselves, acknowledging terror and trauma, as well as love, life, and healing. The song title “Into Each Life Some Rain Must Fall” rings true in the NICU story. I know that we need rain to bring flowers. None of us gets out of here without getting dinged. Trauma brings anxiety and grief, but it also makes us deeper, more compassionate people. Telling stories connects us to other people. We look for life and light in the midst of darkness and pain. I hope that We Are Always With You brings life-giving light.